“My family emigrated out here from Nebraska in the 1920s,” he said. “And we have been farming here ever since. And I’m the first to go into medicine.”
Claassen attended a public high school in Clarkston, then headed to WSU’s Pullman campus for his bachelor’s degree in microbiology and molecular biology. When it came time to apply to medical school, staying in Eastern Washington felt like a no-brainer.
During his time at WSU’s medical school, Claassen had the chance to return to his hometown as part of a WSU clinical rotation in family medicine at TriState Health. “I was working with the team of primary care providers, seeing patients all day long,” he said.
Many of the patients knew him.
Those relationships reflect the medical school’s emphasis on training providers in the communities they already feel connected to and will later serve as part of their medical practices.
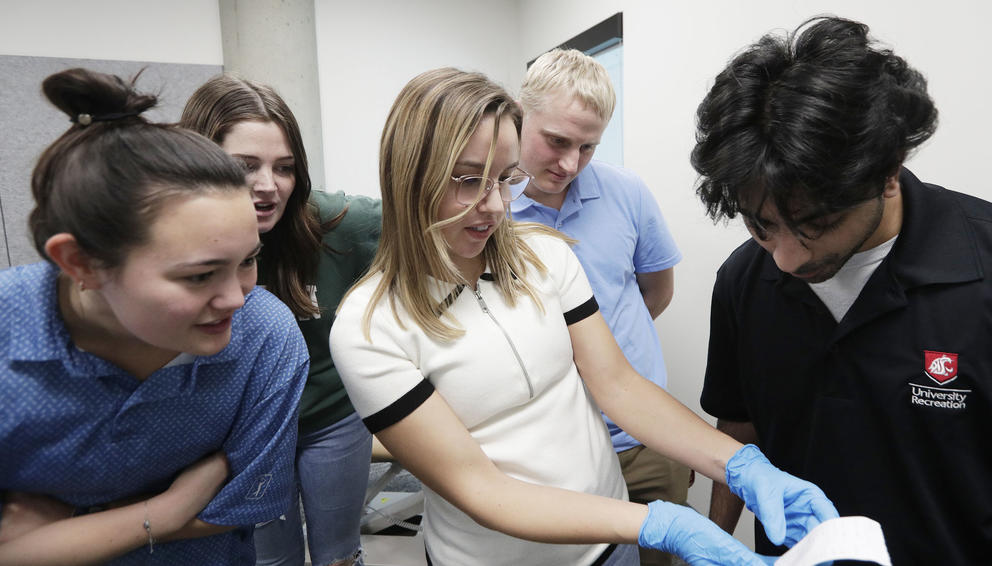
Fourth year medical student Pierce Claassen, seen here doing a mock thyroid exam, will graduate from WSU Medical School later this year. Claassen is the first in his family to go into medicine. He plans to stay in Eastern Washington as he begins his medical career. “There is a profound health care disparity not only across primary care services, but also surgical and subspecialty services,” he said. “We are in need of every single type of physician here in this area.” (Courtesy of Elson S. Floyd College of Medicine)
The 11-year-old Elson S. Floyd College of Medicine is laser-focused on its mission to educate Washington students to become Washington doctors.
Claassen, who’s applying to internal medicine residencies, plans to ultimately pursue gastroenterology and hepatology and work in the region where he grew up — “anywhere from Spokane to Clarkston” — in part because of the entrenched differences in access to medical care he sees between Eastern and Western Washington. “There is a profound health care disparity not only across primary care services, but also surgical and subspecialty services,” he said. “We are in need of every single type of physician here in this area.”
Claassen is repeating the message he has heard repeatedly as a student in the WSU med school: They’re training doctors from the region to serve their neighbors.
“What we’re trying to accomplish here … is to work hard to admit a student body into the College of Medicine who will upon finishing their training go back in higher-than-average numbers to serve those places that are underserved, and those places where we need them the most,” said Ken Roberts, chair of the Medical College’s Department of Translational Medicine and Physiology.
In applying to residencies or fellowships, the three to seven years of training that come after graduation from medical school, medical students have relatively little control over where they’re accepted, so it’s difficult to gauge how well this is working. But according to the Association of American Medical Colleges, about 41% of new doctors practice in Washington if they attended medical school in the state; if they completed their residency here, that number jumps to 70%.
These numbers include Washington’s other, much bigger, public medical school at the University of Washington, which has a long history of educating physicians in the state. The UW School of Medicine was accredited in 1946 and graduated its first doctor in 1950.
“We are happy to have been able to provide a physician workforce since 1950 to serve residents in Washington state,” said Suzanne Allen, vice dean for academic, rural and regional affairs at the University of Washington School of Medicine. “We take great pride in delivering quality care and advancing medical knowledge as an academic healthcare system.”
Of the UW program’s 270 students, over half are from Washington. The medical school also offers training across a five-state region that includes Wyoming, Alaska, Montana and Idaho, with programs focused on rural medicine and underserved communities. Like WSU, the University of Washington also has a mission rooted in health equity, but a very different regional focus.
According to Dr. Leila Harrison, vice dean of admissions, student affairs and alumni relations at the WSU College of Medicine, over a quarter of students in all classes enrolled are from Eastern Washington. All of the school’s students are from Washington, and the majority have childhood connections to the state and obtained their undergraduate degrees here.
Named after former WSU president Elson S. Floyd, the College of Medicine opened in 2017, was fully accredited by 2022, and graduated its first class of 60 students in 2021, who pivoted to online learning during the early months of the COVID-19 pandemic.
The class who entered last fall will be the college’s seventh, and they’ll benefit from lessons learned and resources grown as the program has picked up steam: A new headquarters for the school was dedicated in August 2023, with a building renovation funded by a $15 million allocation from the Legislature. The school also now has over 200 affiliation agreements with hospitals and clinics throughout the state, where students can pursue their clinical rotations in the second half of their training.
The school launched two new residency programs in 2023: a family medicine residency in partnership with Pullman Regional Hospital and a pediatric residency at Spokane’s Providence Sacred Heart Children’s Hospital in partnership with local outpatient pediatric clinics. The family medicine residency, whose funding includes a $2.5 million grant from Premera Blue Cross, accepted its first three residents this past summer.
The pediatric residency, which will welcome its first cohort of students in the summer of 2024, was formed with the intention of addressing disparities in access to health care between children in urban and rural communities.
“As a pediatrician with Providence, I’ve seen firsthand the significant need we have for more pediatricians and pediatric specialties across Eastern Washington,” said Dr. Christian Rocholl, a pediatric emergency medicine physician who will direct the pediatric residency program, in a statement released by WSU when the program was announced in March. “I am thrilled to see this residency program come to fruition, and look forward to leading and training the next generation of pediatricians who will serve our community’s children for years to come.”
The program’s efforts to ensure students continue to practice in Eastern Washington remains largely untested. With only a few classes graduated, it’s still too early to tell how much local output the program will have. But geographical disparities in both access to health care and training for physicians are well-documented: Of the 168 medical residencies and fellowships in Washington, 158 are west of the Cascades, despite the ongoing need for more medical providers in Eastern Washington.
In communities close to the Idaho border, the need for care may be especially acute, since Eastern Washington physicians routinely serve patients from Idaho seeking all kinds of care not broadly available where they live — a need likely to become even greater with the loss of maternity-care providers and ongoing travel related to abortion.
Training physicians in these communities is one way to build capacity, said Roberts, whose involvement goes all the way back to his directorship of a WSU program that preceded the College of Medicine which brought University of Washington medical students to Spokane. That program ended in 2015, but Roberts describes it as “the beginning of a conversation” about opening a medical school at WSU. (UW now has its own medical training facility in Spokane, operated in partnership with Gonzaga University.)
For their first two years, WSU medical students receive training in Spokane. In their second and third years, they have the option of being based at WSU’s locations in the Tri-Cities, Vancouver or Everett, with clinical placements anywhere from the Oregon border to the Olympic Peninsula. (The University of Washington’s clinical placements span its five-state service region.) Among the three classes who have received residency placements and one currently applying, over half the students are pursuing careers in internal medicine, family medicine and general surgery, according to Harrison, the vice dean of admissions.
“As an educational program or college, there’s not that many things you can do to really influence the product you get at the end,” said Roberts. “Students come in and they train for their own reasons, and then they go off and they do the things that they intended to do. But you do have a few points of control. And one of those is the admissions process.”
Currently the College of Medicine admits 80 students annually; all are either Washington state residents or have other connections to the community. “We have a holistic admissions process where we have a bar for baseline qualifications,” said Roberts. If a student has high-enough grades and MCAT scores to be admitted, their application goes through a blind admissions process so that the committee can’t see their grades or scores.
“So they’re making their judgment for admission based on other factors than just straight-up academic performance,” said Roberts. These include where the student grew up, what life experiences they’ve had, and whether — like Claassen, the fourth-year student from Clarkston — they’re committed to seeking work in areas with the greatest need.
That’s the outcome the school is hoping for, and Roberts doesn’t think it means competing with other medical schools. “The state of Washington is well under the average in almost all of our counties for the number of physicians, and health care access in general,” he said. More training opportunities can change that: “It’s more capacity for educating physicians and an effort to do that in a way that puts more physicians where we need them.”
The College also partners with federally qualified health centers and rural clinics, and has built discussions about health equity and social determinants of health into its curriculum, contextualizing the health disparities students observe across the state.
“Medical schools are complicated and wonderful entities,” said Roberts, and with time, he’s confident the College of Medicine will grow. “Given enough support over enough years, it will begin to look something like the University of Washington,” he said. “The University of Washington is nearly 100 years old, so it’s had a huge head start.”
Ultimately, Roberts hopes that having a second public medical school will broaden access to health care across the state and more accurately reflect the size and needs of Washington communities beyond urban hubs like Seattle. “We have almost eight million people,” he said. “We can do two medical schools.”
CORRECTION: This version of the story corrects the amount of money the family medicine residency program received from Premera Blue Cross and corrects the spelling of Dr. Christian Rocholl's name.